Contact Exams
Corneal Staining During Contact Lens Exams
FSDAVCFEBFEVSDDVFSD
FSDAVCFEBFEVSDDVFSD
FSDAVCFEBFEVSDDVFSD
What Corneal Staining Actually Means
What is corneal staining? It is a pattern your eye doctor sees after placing a safe dye, usually fluorescein, on the eye during a contact lens exam. The dye highlights tiny areas where surface cells are stressed or disrupted, showing where the cornea may be dry or irritated. This creates a clear picture.
Corneal staining contact lenses patients hear about does not always mean serious damage, but it explains symptoms like burning, fluctuating vision, and light sensitivity. During a contact lens exam staining evaluation, your optometrist can adjust lenses early so minor irritation does not develop into a larger corneal problem for term eye health.
What is corneal staining? It is a pattern your eye doctor sees after placing a safe dye, usually fluorescein, on the eye during a contact lens exam. The dye highlights tiny areas where surface cells are stressed or disrupted, showing where the cornea may be dry or irritated. This creates a clear picture.

Corneal staining contact lenses patients hear about does not always mean serious damage, but it explains symptoms like burning, fluctuating vision, and light sensitivity. During a contact lens exam staining evaluation, your optometrist can adjust lenses early so minor irritation does not develop into a larger corneal problem for term eye health.

Common Causes in Contact Lens Wearers
Dryness is the most common cause of corneal staining contact lenses patients experience. When the tear film breaks up too quickly, the cornea loses its smooth protective layer. Each blink increases friction, especially if a lens is slightly tight, worn too long, or not well matched to tear quality. Solution sensitivity may also play a role, as certain preservatives can irritate the ocular surface over time.
Lens deposits, inconsistent cleaning habits, and sleeping in lenses increase risk. Makeup debris, environmental airflow, and allergy-related eye rubbing add additional stress. In some cases, contact lens fit irritation creates a repeatable staining pattern where the lens edge interacts with the cornea or surrounding tissue. These patterns are helpful clues that guide specific adjustments.
Your doctor evaluates location (central or peripheral), density, and whether one eye is more affected. Dry eye corneal staining may appear as scattered areas across the surface, while mechanical irritation often forms a distinct shape. A thorough eye doctor contact lens evaluation Houston patients schedule regularly helps determine whether the cause is tear instability, lens fit, overwear, solution reaction, or a combination of factors.
How Doctors Grade and Interpret Staining
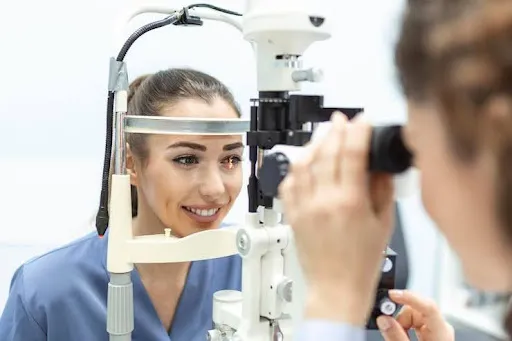
Doctors grade staining based on location, severity, and pattern. Mild, scattered staining may reflect extended screen time or temporary dryness. Denser or localized staining can suggest mechanical irritation, debris trapped under the lens, or lens edge interaction. An inferior band of staining often indicates exposure-related dryness, while a specific spot may raise concern for abrasion risk. These visual clues guide early clinical decisions for patient comfort and long term care.
Findings are interpreted alongside symptoms and tear film testing. If symptoms are mild but staining is significant, prevention becomes the focus to protect long-term corneal health.

If symptoms are strong but staining appears mild, nerve sensitivity, allergy, or tear instability may require broader dry eye treatment rather than lens changes alone. This approach ensures balanced care for comfort and vision stability over time and supports lasting ocular surface health goals.
Staining is always reviewed with other measurements such as tear breakup time, lid margin health, and lens surface quality to give a complete picture of ocular surface performance. Two patients can have staining but require completely different solutions based on lifestyle, environment, and tear stability. Follow-up visits confirm whether clinical changes are truly improving the surface rather than simply masking discomfort temporarily. This ongoing evaluation helps ensure that treatment decisions support both comfort and long-term eye health instead of providing only short-term relief.
If staining continues despite adjustments, your doctor may recommend a more proactive strategy. Options may include daily disposable lenses, switching to a different lens material, or using modified wear schedules to minimize surface stress. In many cases, targeted dry eye treatment is added to reduce friction and stabilize the tear film. These combined steps aim to restore balance to the ocular surface, improve lens tolerance, and prevent small surface disruptions from developing into more serious corneal complications over time.
Fixes That Usually Help Quickly
Many cases improve with simple steps such as shortening wear time, improving cleaning technique, switching solutions, and adding preservative-free lubricating drops. If contact lens fit irritation is contributing, adjusting the lens curve, diameter, or material often reduces friction quickly and restores comfort. A temporary glasses break can also allow the surface to heal before resuming lens wear, helping prevent further stress on sensitive tissue and supporting natural recovery of the eye.
When dryness drives staining, consistent lid hygiene and warm compresses help improve oil gland function and tear stability. Persistent cases may require prescription anti-inflammatory drops or a structured dry eye treatment plan. The goal is both healing the corneal surface and eliminating the trigger so staining does not return, ensuring long-term comfort, clearer vision, and safer contact lens use over time.
When Staining Is a Bigger Warning Sign
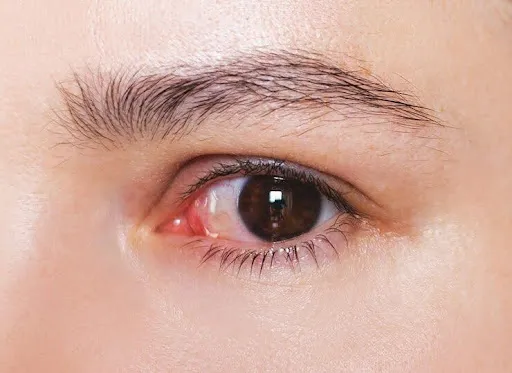
Staining becomes more concerning when it is dense, painful, associated with light sensitivity, or accompanied by discharge. These symptoms may indicate abrasion, infection risk, or significant inflammation that requires prompt professional care. When several warning signs appear together, they suggest the corneal surface is under stress and should not be ignored.
If you experience sharp pain, sudden persistent blur, or a very red eye, stop wearing lenses immediately and seek an eye exam. Early intervention protects your cornea and reduces the chance of complications that could threaten vision and comfort.
Staining becomes more concerning when it is dense, painful, associated with light sensitivity, or accompanied by discharge. These symptoms may indicate abrasion, infection risk, or significant inflammation that requires prompt professional care. When several warning signs appear together, they suggest the corneal surface is under stress and should not be ignored.
If you experience sharp pain, sudden persistent blur, or a very red eye, stop wearing lenses immediately and seek an eye exam. Early intervention protects your cornea and reduces the chance of complications that could threaten vision and comfort.

Repeated staining despite good hygiene may signal underlying dry eye disease, allergy, or a mismatch between your lens design and your ocular surface. A thorough evaluation ensures the root cause is identified and properly addressed for lasting eye health.
How Clinics Prevent Staining From Coming Back
Prevention begins by matching lenses to your actual ocular surface needs. Your optometrist may refine lens parameters, switch materials, or recommend a replacement schedule that limits deposits and reduces irritation. Daily disposables reduce residue-related staining because each lens starts clean and free from buildup. For reusable lenses, proper rubbing, thorough rinsing, and regular case replacement are essential to maintain lens surface quality and protect the cornea from unnecessary stress and contamination during routine wear.
Dry eye prevention is often central to the management plan. Evaluating tear stability, gland function, and inflammation helps guide recommendations such as warm compresses, lid cleansers, preservative-free tears, and environmental adjustments. Allergy treatment may also reduce rubbing and surface stress that worsen staining patterns. In more advanced situations, specialty designs like scleral lenses may be considered to provide continuous hydration and reduce friction on the ocular surface.
Follow-up ensures real improvement rather than temporary symptom relief. Your doctor may schedule a recheck after lens or treatment changes to confirm reduced staining and improved tear stability over time. These visits help verify that the surface is healing and that comfort is sustained throughout normal wear hours. If staining persists, adjustments continue until the ocular surface remains stable and resilient during everyday activities.
Lens comfort functions as a system in which wear time, screen habits, environment, lid health, and lens type all interact. No single factor works alone. When these elements are aligned properly, staining often resolves and contact lenses feel consistently comfortable again. This integrated approach supports long-term corneal health, better visual clarity, and safer contact lens use for patients with sensitive or dryness-prone eyes.
Questions to Ask at Your Next Exam
Ask, “Where is the staining located, and what does that pattern suggest?” Understanding cause and effect turns concern into a clear action plan. Clarify whether dryness, contact lens fit irritation, solution sensitivity, or overwear is most likely responsible and which change should come first. This helps target the main trigger instead of making random adjustments.
Discuss safe wear time while healing by asking, “Should I take a glasses break?” and “How often should I use contact-safe drops?” If dryness is present, confirm which lubricants are compatible with your lenses. If lid inflammation or allergies are contributing, ask what daily routine will best support recovery and reduce surface stress.

Ask, “Where is the staining located, and what does that pattern suggest?” Understanding cause and effect turns concern into a clear action plan. Clarify whether dryness, contact lens fit irritation, solution sensitivity, or overwear is most likely responsible and which change should come first. This helps target the main trigger instead of making random adjustments.
Discuss safe wear time while healing by asking, “Should I take a glasses break?” and “How often should I use contact-safe drops?” If dryness is present, confirm which lubricants are compatible with your lenses. If lid inflammation or allergies are contributing, ask what daily routine will best support recovery and reduce surface stress.
Finally, ask about warning signs and follow-up timing. Knowing when to stop lenses and call—pain, discharge, persistent blur, or light sensitivity—protects your cornea. Clear recheck scheduling ensures the staining is resolving, not recurring.
What to Do After You’re Told
If your doctor identifies corneal staining, treat it as helpful information rather than a reason to panic. Follow recommendations carefully: reduce wear time, switch solutions if advised, and use contact-safe lubrication consistently to support healing. Avoid sleeping in lenses, replace cases as directed, and allow your eyes a short recovery period if needed. These simple steps help calm surface irritation and prevent minor problems from becoming more serious. Staying consistent with care routines protects the cornea and improves overall comfort during daily lens wear.
If you develop worsening redness, pain, discharge, or light sensitivity, stop lens wear and Contact us promptly at Kleinwood Vision for guidance. With the right adjustments and a thorough eye doctor contact lens evaluation Houston patients trust, most people return to safe, comfortable lens wear with healthier corneal surfaces and improved long-term eye health.

Contact Info
Hours of Operation
Mon - Fri | 9:00 AM - 5:00 PM
Sat - Sun | Closed
Holiday Hours: We are closed for the following holidays: New Years Day, Memorial Day, Independence Day, Labor Day, Thanksgiving Day, Christmas Day
The information provided on this website is for general informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the guidance of a licensed eye care professional or qualified health provider with any questions you may have regarding a medical condition or vision concern. Results from eye care services may vary by individual.
© 2026 Kleinwood Vision. All rights Reserved.


